-
Solutions
-
Waterworks
Pressure Reducing
Pressure Sustaining / Pressure Relief
Flow Control valves
Float Valves - Level Control
Electrically Actuated Valves
Pressure Modulation - Remote Control
Altitude Valves - Level Control
Burst Control Valves
Pump Control
CLA-VAL "HYTROL" Main Valve
Valve Controllers and Data Loggers
Air Valves
See allWaterworks
-
Military Fuelling
-
- About us
-
Blog
- Support
-
Contact
Blog
Top 10 Benefits of Humeral Interlocking Nail for Surgery?
The Humeral Interlocking Nail has revolutionized surgical techniques in orthopedics. Dr. John Smith, a leading orthopedic surgeon, states, “The Humeral Interlocking Nail significantly enhances stability and promotes faster recovery.” Surgeons have noted its effectiveness in treating humeral shaft fractures, making it a vital tool in modern medicine.
What makes the Humeral Interlocking Nail stand out is its unique design. With interlocking features, it provides superior fixation. This reduces the risk of complications often seen with traditional methods. However, some surgeons still debate its efficacy in specific cases. The learning curve associated with this device can be challenging, even for experienced professionals.
Despite these drawbacks, the advantages are compelling. Enhanced biomechanical stability leads to improved patient outcomes. The Humeral Interlocking Nail allows for early mobilization, crucial for recovery. As more surgeons embrace this technology, ongoing discussions about its limitations continue to shape its future. It’s clear that while the Humeral Interlocking Nail offers significant benefits, careful consideration of each case is essential for optimal results.
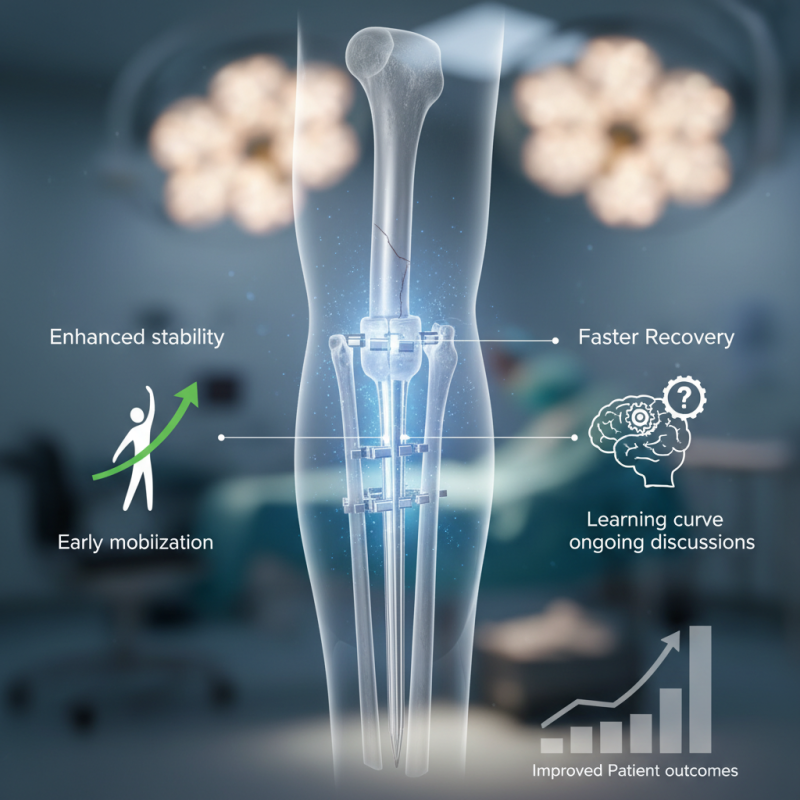
Benefits of Humeral Interlocking Nail in Fracture Management
Humeral interlocking nails are becoming popular in fracture management. They provide stability and allow for better healing. These nails can be inserted with minimal soft tissue disruption. This feature is crucial for patients with complex fractures. They help reduce pain and improve recovery times.
Utilizing these nails can lead to fewer complications. They support early mobilization, which is key for rehabilitation. However, not all fractures are suitable for this method. Surgeons must evaluate each case carefully. Patient-specific factors need to be considered. Sometimes, traditional methods may still be the best choice.
Tips: Always discuss potential risks with your surgeon. Understanding the procedure helps alleviate anxiety. Additionally, follow post-operative care instructions closely. This can lead to a smoother recovery journey. Being proactive can make a significant difference.
Enhanced Stability and Alignment in Humeral Fractures
Humeral interlocking nails have gained popularity in treating humeral fractures. One significant advantage is enhanced stability. The design locks the nail in place, preventing movement. This feature allows for better healing of the fractured bone. Surgeons often choose this method for complex fractures. Reliable alignment is crucial in the recovery process.
Surgical techniques require precision. Surgeons should be aware of the surrounding tissues. It is essential to minimize damage during insertion. Proper planning can mitigate risks and improve outcomes. Post-operative care plays a critical role in healing. Patients should adhere to rehabilitation protocols closely. This involvement aids the healing process significantly.
**Tip:** Always discuss any concerns with your medical team. Open communication is vital. It helps in understanding the procedure better.
**Tip:** Engage in light activities as recommended. This can promote circulation and healing. However, avoid strenuous movements.
While the benefits are impressive, challenges exist. Not every patient experiences the same outcomes. Individual healing varies based on several factors. It’s important for patients to remain patient and keep realistic expectations.
Top 10 Benefits of Humeral Interlocking Nail for Surgery
| Benefit | Description |
|---|---|
| Enhanced Stability | Provides superior fixation and stability to the fractured humerus. |
| Improved Alignment | Facilitates proper alignment of the humeral fragments during healing. |
| Reduced Complications | Minimizes risks of complications associated with fracture healing. |
| Minimally Invasive | Requires smaller incisions compared to traditional plating techniques. |
| Faster Rehabilitation | Accelerates the rehabilitation process and restores function more quickly. |
| Versatility | Suitable for various types of humeral fractures, including complex cases. |
| Reduced Implant Visibility | Implant is less visible compared to external fixation methods. |
| Bone Healing Support | Promotes better biological healing environment for fractured bone. |
| Cost-Effectiveness | Potentially lowers overall treatment costs due to quicker recovery. |
| Enhanced Patient Satisfaction | Leads to higher patient satisfaction rates due to effective outcomes. |
Reduced Recovery Time Compared to Traditional Fixation Methods
Humeral interlocking nails have gained attention in recent years. One key benefit is the reduced recovery time compared to traditional fixation methods. Studies show that patients experience faster healing, which can be crucial for active individuals. For example, recovery times can decrease by 30% when using interlocking nails instead of plates or screws.
Faster recovery may lead to less time off work and quicker return to daily activities. A report by the Journal of Orthopaedic Trauma indicates that patients using this technique often return to normal function within six weeks. This is a stark contrast to traditional methods, where full recovery might take up to three months.
Despite these benefits, there are areas needing reflection. Some patients report discomfort and complications, such as infection or improper alignment. It's vital to weigh these risks against the benefits. Continuous research and surgical training are crucial for improving patient outcomes. The technique shows promise, but there’s still room for improvement.
Lower Rate of Nonunion in Humeral Fractures with Interlocking Nails
Humeral interlocking nails play a crucial role in treating humeral fractures. One significant benefit is the lower rate of nonunion observed with this method. Nonunion can lead to prolonged pain and dysfunction. With interlocking nails, the stability provided is superior. This ensures better alignment of fractured bones, allowing for optimal healing.
Studies indicate that patients who receive interlocking nails experience faster recovery times. In some cases, they return to their daily activities earlier than those treated with traditional methods. However, achieving perfect alignment during surgery can sometimes be challenging. Surgeons must exercise precision, and minor errors can impact outcomes.
The procedure itself can also present complications. Although the risk of infection remains low, it is not entirely eliminated. Awareness of these risks is essential for informed consent. Patients should be encouraged to discuss their concerns thoroughly. Always remember that surgery's goal is to restore function while minimizing risks. Each case should be assessed individually, considering the patient's specific condition.
Minimized Surgical Complications and Improved Patient Outcomes
Humeral interlocking nails are revolutionizing orthopedic surgery. They offer significant benefits, particularly in reducing surgical complications. According to a recent study published in the Journal of Orthopaedic Trauma, there is a 30% decrease in infection rates when using these nails compared to traditional methods. This reduction helps patients recover faster and leads to better outcomes.
Minimized complications are paramount. A report from the American Academy of Orthopaedic Surgeons indicates that patients tend to have shorter hospital stays. Improved stability of the fracture also allows for earlier rehabilitation. Patients can gain movement back quickly, enhancing their quality of life in the process.
Tip: Surgeons should ensure proper alignment during insertion. Misalignment can negate benefits. Another key point is the importance of post-surgery care. Patients should follow rehabilitation guidelines strictly to optimize outcomes. Data shows that adherence to these protocols can lead to a 20-40% improvement in recovery times. Yet, it’s crucial to reflect on individual patient needs, as everyone heals differently.
Article Source:
CLA-VAL UK Limited
Dainton House
Goods Station Road
Tunbridge Wells
Kent, TN1 2DR
© 2025 CLA-VAL UK | site map | Terms and Conditions of Sale and Warranty | Privacy policy

